Neck pain that travels into the shoulder, arm or hand can wear you down in a way that is hard to explain until you live it. When symptoms and imaging point to a worn or unstable cervical segment, cervical spinal fusion may help by taking painful motion out of that level and restoring stability.
In simple terms, cervical spinal fusion is a procedure that allows two neck vertebrae to heal together as one solid unit, creating a more stable foundation for the surrounding nerves and spinal structures.
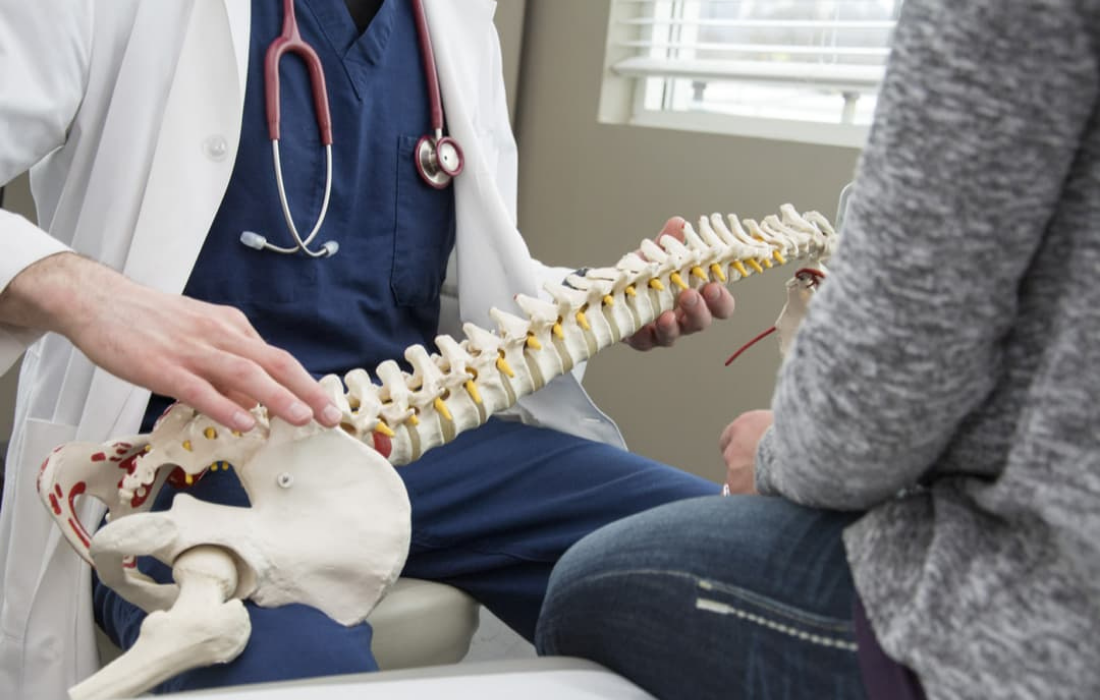
Anatomy of the Neck
Your neck supports the head while still allowing a wide range of motion. That balance comes from seven cervical vertebrae, discs between most levels and supporting facet joints, ligaments and muscles that protect the spinal cord and nerve roots.
Nerves exit the spine through foramina. If a disc herniates, bone spurs form or the space narrows, those nerves can get irritated. People often notice arm pain, numbness, tingling or weakness, sometimes with grip changes.
What Is Cervical Spinal Fusion Surgery?
Fusion is a controlled way to help two vertebrae heal into one solid unit. Cervical spinal fusion aims to stabilize the segment after the surgeon removes the source of nerve or spinal cord compression and to reduce painful movement at that level.
A common form is anterior cervical discectomy and fusion (ACDF). Cleveland Clinic estimates that about 132,000 people in the United States have ACDF each year.
How This Procedure Is Performed
Surgeons choose the approach based on where compression sits, which levels need treatment and what stability the spine needs afterward. You receive general anesthesia and the team confirms the correct level with imaging.
In cervical spinal fusion, surgeons follow the same core steps across most techniques:
- Access the spine through a small incision and move aside nearby tissues
- Remove the damaged disc or bone spurs that press on nerves
- Prepare the bone surfaces
- Place a spacer or bone graft material between the vertebrae
- Add stabilization hardware such as plates, screws or rods when appropriate
With anterior cervical spinal fusion, the incision sits in the front of the neck. Surgeons often remove the disc first, place a graft or cage, then secure the area with a plate and screws to support alignment while fusion develops. With posterior cervical spinal fusion, the incision sits in the back of the neck, and the stabilization strategy can differ based on the problem and the anatomy.
Procedure time varies, but spinal fusion operations commonly take around three to four hours.
Who Is a Candidate for Cervical Spinal Fusion Surgery?
Most people start with nonsurgical care. Surgery enters the conversation when symptoms continue, worsen or cause neurologic problems that show up on an exam and match what imaging shows.
Cervical spinal fusion is more likely when the spine needs added stability after decompression or when a segment already shows instability. Common reasons include:
- Arm symptoms that do not improve with a structured care plan
- Signs of spinal cord compression, such as balance changes, hand clumsiness or trouble with fine motor tasks
- Degenerative changes, stenosis or bone spurs that compress nerves
- Trauma, tumor or infection that compromises spinal stability
Your surgeon weighs imaging, neurologic findings, health history and goals. In some cases, they may also discuss motion-preserving alternatives such as cervical disc replacement.
Cervical Spinal Fusion Recovery
After cervical spinal fusion, recovery has a fast part and a slow part. Pain control and safe mobility improve early, while bone healing takes longer and drives activity restrictions. Many patients go home the next day after common cervical fusion pathways, though some plans include a longer stay based on complexity and medical factors.
A realistic timeline for cervical spinal fusion recovery often looks like this:
- First 2 Weeks: Short, frequent walks, incision care and a follow-up visit
- Weeks 4 to 6: Gradual return to routine tasks, then start rehab if cleared
- Months 3 to 4: Stronger healing, still with limits on heavier lifting
- Up to 12 months: Fusion continues to mature
Temporary swallowing discomfort or voice changes can happen after anterior approaches. Some people use a collar for support. Nicotine can slow healing and raise complication risk, so surgeons often ask patients to stop well before surgery and avoid smoking during recovery.
Infection after ACDF is extremely uncommon, reported as less than 1 in 1,000 cases.
A Spine Team That Treats the Whole Picture
If you are considering cervical spinal fusion, the details matter. Approach choice, implant selection and the recovery plan should match your diagnosis and your life.
At University Orthopaedic Associates (UOA), patients can access fellowship-trained spine surgeons and a full range of cervical procedures, including cervical spinal fusion and related options like ACDF or cervical disc replacement. Our surgeons have performed more than 8,500 spine procedures.
If you would like to discuss your symptoms with a spine surgeon, you can request an appointment here.