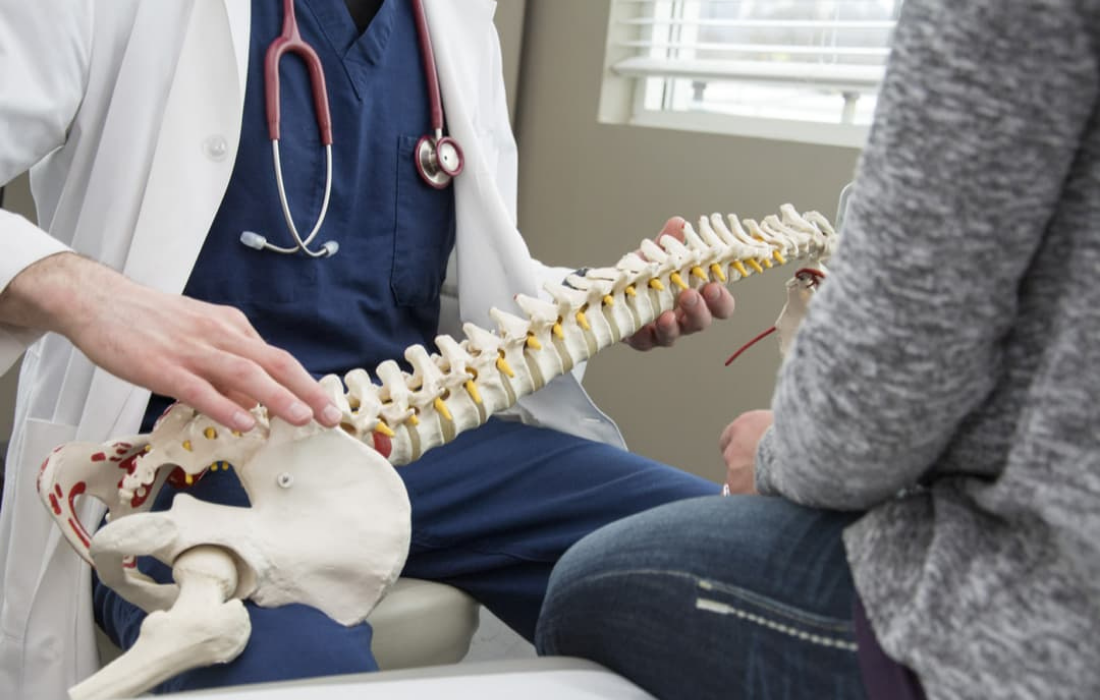
Degenerative conditions of the spine—also known as degenerative spine disease—refer to the damage that occurs over time to the vertebrae in the cervical (neck) or lumbar (back) spine. Vertebrae are small bones that make up the spine and house the spinal cord.
In the case of the neck, degenerative spine disease impacts the seven vertebrae that make up the upper region of the spine. In the back, it is the five (in some people six) vertebrae that comprise the lower region of the spine.
As we age, the stresses endured by the spine have their impact——often on the cushioning discs between vertebrae, causing them to become weaker and drier and thus more prone to damage and deterioration. This deterioration can also affect the various muscles and ligaments that make up the spine.
Types of Degenerative Spine Disease
There are a number of conditions associated with degenerative spine disease. Below are the most common:
Osteoarthritis. Osteoarthritis is the deterioration of the cartilage in the facet joints of the spine. When that cartilage wears down, it results in bone-on-bone contact within the joints.
Herniated or bulging disc. The disc between vertebrae are made up of a soft, jelly-like center surrounded by a tough exterior. Herniation occurs when the soft center leaks through a crack in the exterior and places pressure on a nearby nerve, nerve roots or the spinal canal.
Bone spurs. These are protrusions of bone that occur with deterioration caused by arthritis. They can become a problem if they come into contact with a nearby nerve.
Spinal stenosis. Stenosis, a word that means the narrowing of the spinal canal, generally occurs in both the cervical or lumbar spine. It is most commonly caused by bulging or herniated discs, bone spurs and spondylolisthesis.
Spondylolisthesis. This condition occurs when one of the vertebra slides forward and onto the bone below it. This condition can be graded low or high, depending on the amount of slippage of the vertebrae. When the forward slippage is over 50 percent, it is considered high-grade.
Degenerative scoliosis. This is the most common type of scoliosis in adults and usually happens in the lumbar (lower) spine. Also referred to as adult onset scoliosis, it is caused by degeneration of the discs and facet joints of the spine. It results in an abnormal side-to-side curvature of the spine.
Other causes of degenerative spinal disease can include:
- Alcohol abuse
- Benign tumors
- Cancer
- Infections
- Obesity or overweight
- Osteoporosis
- Rheumatoid arthritis
- Smoking
- Strenuous, repetitive movement
Symptoms
Depending on the location of the problem, some symptoms may vary. Common symptoms include:
- Pain (chronic or sharp, with movement or without)
- Limited motion
- Deformity of the spine
If there is damage or injury to the nerves, additional symptoms can include:
- Numbness, tingling or weakness
- Bladder and bowel dysfunction
- Sexual dysfunction
Diagnosis
In addition to a review of symptoms with your doctor, he or she will likely perform a physical exam, particularly of the painful areas, as well as a neurological exam (to check for muscle function and reflexes). In addition, the diagnosis of degenerative spine disease is enabled by the following tests:
- X-ray of the spine
- Magnetic resonance imaging (MRI) to evaluate the spinal canal, discs and nerves
- Computed tomography (CT) scan, possibly used in the event of the need for clarification or to rule out another cause
- Discogram, a study to determine damaged spinal discs
Treatment
Treatment of degenerative spine disease begins with conservative measures. Depending on the location and severity of symptoms, these measures may include:
- Rest
- Ice and/or heat therapy
- Lifestyle modification
- Over-the-counter pain medications
- Exercise/physical therapy
- Pain management techniques (e.g., steroid injections, epidural)
If these measures no longer provide relief, and/or the condition is more severe, surgery may be indicated. At University Orthopaedic Associates (UOA)—among our many spine procedures—we specialize in minimally invasive spine surgery, which offers benefits including:
- Outpatient (same-day) surgery
- Reduced risk of complications
- Reduced blood loss
- Less disruption of surrounding muscles and tissue
- Less post-operative pain
- Shorter recovery time
- Reduced risk of scarring
For a thorough and customized evaluation and treatment plan for spine conditions and other orthopaedic needs, contact University Orthopaedic Associates (UOA).